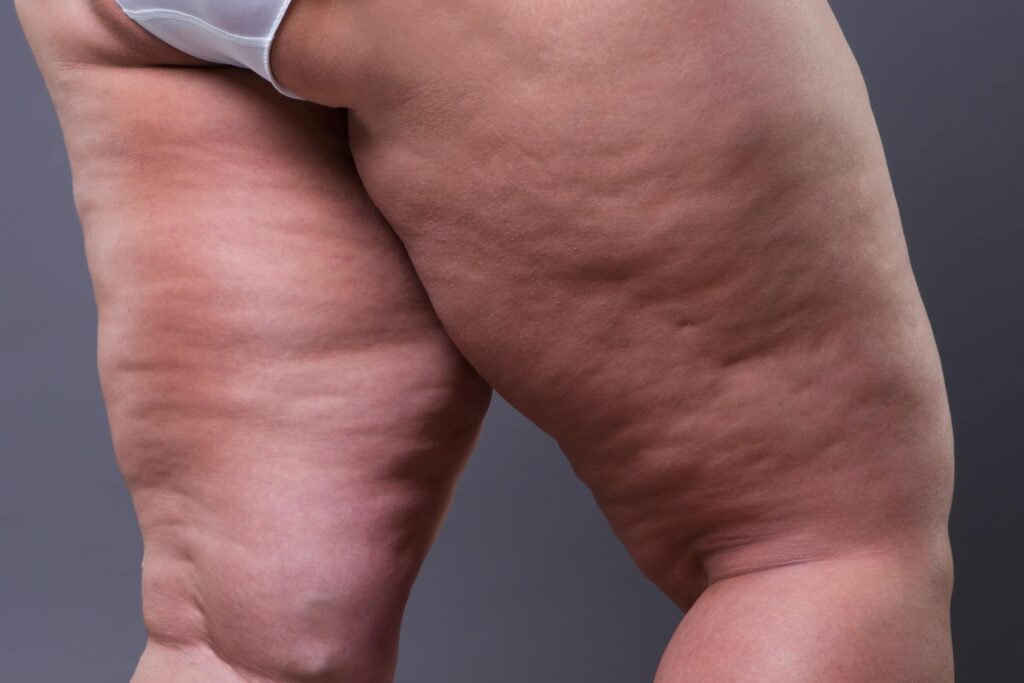
Key Takeaways
- Lipedema fat is resistant to traditional weight loss methods, so dieting alone is unlikely to shrink affected areas.
- Hormonal influences and chronic inflammation play a role in lipedema fat accumulation and symptom severity.
- Because lipedema is frequently misdiagnosed, the correct diagnosis is critical.
- Targeted nutrition plans that emphasize anti-inflammatory foods and lymphatic support can assist in managing symptoms and enhance overall health.
- Both gentle exercise and compression therapy play significant roles in reducing swelling, supporting mobility, and enhancing quality of life.
- Taking care of both your physical and emotional health, including support from professionals and support groups, is the key to well-rounded lipedema care.
Lipedema legs won’t diet away because lipedema is a chronic fat disorder. There are many patients who observe that, despite rigorous diet and exercise, the shape and size of their legs remain unchanged.
Lipedema typically presents in women and can present with pain, swelling, or easy bruising. For the full scoop on how lipedema works and what helps, read on.
The Stubborn Fat
Lipedema fat behaves unlike regular fat. It accumulates in the legs, hips, and occasionally arms, but it refuses to diminish with conventional weight loss techniques. This stubborn fat is shaped by specialized cell structure, hormones, inflammation, lymphatic problems, and genetics.
1. Cellular Structure
Lipedema fat cells are larger than normal fat cells and like to group together. They bunch up in clusters and develop thick pads beneath the skin, which can make the legs appear bulky — even if the rest of the body is slim.
The fat accumulates symmetrically, so both legs appear identical. Within them is more fibrous tissue than usual fat. This fibrous tissue is like a web, turning the fat harder and less likely to shrink with diet or exercise.
Unlike regular body fat, lipedema fat remains even if you lose kilos somewhere else. Others experience that the fat is lumpy, flabby, or even sore. Lipedema fat has different cell makeup which affects health. That can impede circulation and cause bruising.
Sometimes, the skin over these areas becomes sensitive.
2. Hormonal Influence
Hormones, particularly estrogen, have a strong hand in why lipedema fat accumulates. Estrogen can direct the body to store fat in the hips and legs, which coincides with where lipedema appears. Insulin, the other hormone, can drive your body to hang on to more fat.
Puberty, pregnancy, or menopause can all lead to hormonal changes that frequently exacerbate lipedema. That’s why so many individuals observe initial indications of lipedema during these phases.
Fixing or balancing hormones is not easy, but it’s relevant when considering treatment options.
3. Chronic Inflammation
This chronic inflammation means the body’s tissues remain irritated. With lipedema, this can cause leg pain, swelling, and a heaviness in the legs. Some foods like sugar or processed fats worsen inflammation.
Keep moving, skipping the foods and anti-inflammatory treatments can reduce symptoms. Maintenance is crucial because inflammation can return.
4. Lymphatic Dysfunction
The lymphatic system circulates fluid through the body. When it doesn’t work well, fluid accumulates in the legs, resulting in increased swelling and pain. Lipedema fat might press on lymph vessels, making matters even worse.
Symptoms are swelling, skin alterations, and heaviness. Special treatments such as manual lymphatic drainage or compression can assist in shifting fluid out and easing discomfort.
5. Genetic Predisposition
Lipedema is frequently hereditary. Most lipedema patients are female, with many able to trace a mother or sister exhibiting similar signs. Genetics can influence the manner in which fat is stored and its location.
Heading into your family history can help with early diagnosis and better management options. There are some genetic markers being researched, but a lot remains a mystery.
Beyond The Scale
One cannot glance at a scale to get the whole story with lipedema. This chronic fat condition primarily impacts females and is commonly misdiagnosed as obesity or something else. Regular dieting causes regular fat cells to shrink, but since lipedema tissue is tough and unyielding, it does not shrink.
While weight loss may reduce pain and progression, the abnormal fat associated with lipedema tends to remain. Controlling overall weight, particularly abdominal, keeps symptoms in check because the more belly fat there is, the worse the disease can become. Measuring body composition and fat distribution is more valuable than just recording weight.
Managing lipedema requires more than a diet plan. It requires a combination of medical treatment, lifestyle modifications, and occasionally, surgery.
Misdiagnosis
Lipedema is commonly mistaken for obesity or lymphedema. The symptoms can resemble swollen legs, simple bruising, and hard-to-lose fat that won’t deflate with calorie reductions. Too many patients end up on starvation diets and exhausting exercise programs without seeing their legs return to normal.
This often causes frustration, shame, and delays the pursuit of proper treatment. A bad diagnosis results in bad treatment and worse health. For instance, individuals might be advised to continue shedding weight even as the fat on their legs lingers.
This fixation on weight can overlook the pain, swelling and mental stress lipedema inflicts. Some might even be burdened with peg treatments that don’t suit them. Educating healthcare providers is critical to reducing the rate of misdiagnosis.
Most doctors aren’t trained to recognize lipedema, so raising awareness helps ensure more patients receive proper treatment. Patients need to feel comfortable questioning and seeking second opinions if their experience doesn’t align with what they’re being told. Self-advocacy may ultimately aid you in securing an accurate diagnosis and improved treatment.
Diagnostic Tools
Diagnosing lipedema begins with a physical exam. A doctor checks for classic signs: legs with a column-like shape, fat that feels soft and spongy, and pain with touch. Imaging, such as ultrasound or MRI, can demonstrate fat distribution and exclude other etiologies.
A thorough medical history still counts. Doctors should inquire about family history, pubertal or pregnancy changes, and pain or swelling. These particulars distinguish lipedema from other fat or lymph issues.
Specialized healthcare providers, such as those in vascular medicine or lymphology, tend to receive more education in identifying lipedema. They apply fixed standards, such as those created by global lipedema organizations, to assist in formulating a definitive diagnosis.
Applying these criteria, combined with education and appropriate technology, increases the likelihood of early recognition of lipedema and provides patients with a defined treatment roadmap.
A New Food Philosophy
Transitioning to a new food philosophy for lipedema is about caring less about calorie limits and more about feeling well. Science underscores how conventional dieting almost never causes lipedema legs to shrink, as the implicated fat tissue acts different from typical body fat. Instead, it is about eating to nourish and alleviate symptoms, selecting foods that combat inflammation, harmonize fluids, and sustain energy.
Whole foods offer a foundation. Non-starchy vegetables, legumes, fruits, and whole grains, think Mediterranean-style, deliver fiber, vitamins, and minerals that promote health and can aid in controlling lipedema. Good fats, such as olive oil and fatty fish, can be incorporated into meals daily for additional advantages.
Some experiment with keto or low-carb, consuming less than 100 to 150 grams a day, while others find a Mediterranean or RAD diet more sustainable due to its higher fiber and wider nutrient profile. Refined grains and sugars are wise to steer clear of because they can spark symptom flare-ups in some individuals.
- Make non-starchy vegetables (broccoli, spinach, peppers) the mainstay of every meal.
- Add healthy fats like olive oil, avocado, and nuts.
- Restrict added sugars and white flours like white bread and pastries.
- Include legumes and whole grains if tolerated.
- Prioritize fresh, unprocessed foods over packaged options.
Personalized nutrition is the way. What works for one doesn’t work for another, so it’s useful to customize meal plans to suit particular needs, tastes, and tolerances.
Anti-Inflammatory Eating
One of the underlying issues of lipedema is chronic inflammation, so anti-inflammatory eating is a great asset. Berries, leafy greens, nuts, seeds, olive oil, and fatty fish all help tamp down inflammation. It is vital to avoid processed and high-sugar or trans-fat foods, as these can aggravate symptoms.
- Berries such as blueberries and strawberries are high in antioxidants and vitamins and help lower inflammation.
- Leafy greens (spinach, kale) are packed with phytonutrients and support immune balance.
- Fatty fish (salmon, mackerel) are rich in omega-3 fatty acids and are proven to ease inflammatory markers.
- Olive oil contains oleocanthal, which acts like a natural anti-inflammatory.
- Nuts and seeds are good sources of healthy fats and antioxidants.
Meal planning can assist. Prepping anti-inflammatory meals in advance simplifies healthy decisions. Experimenting with other plans, like a Mediterranean or modified keto diet, allows patients to discover what best suits their bodies and symptom profile.
Others may do better with more fiber, while still others may do better with fewer carbs.
Lymphatic Support
Cucumber, celery, and watermelon are examples of foods that nourish fluid balance and support the lymphatic system. Sufficient protein from fish, lean meats, or plant-based sources provides form to tissues and can help any swelling subside. Citrus and berry flavonoids aid lymph flow, so they are wise daily picks.
Hydration is non-negotiable for lymphatic health. If you drink enough water, around 2 liters per day for most adults, it will flush excess fluid from tissues and keep natural drainage flowing. Certain patients discover that natural teas, like dandelion or nettle, may provide gentle diuretic effects and alleviate bloating.
Supplements such as vitamin C, rutin or horse chestnut may be used, but it’s best to discuss these with a health professional first. Monitoring what goes in and how the body reacts helps individuals identify trends, modify their consumption, and control symptoms.
Movement That Heals
For lipedema patients, dieting-induced weight loss rarely affects the size of the legs. Instead, soft movement is at the core of symptom management, enhancing daily function and improving mood. Movement, with care, keeps the body strong and the mind resilient even if it doesn’t reduce the leg fat.
Gentle Exercise
Delicate activities like easy walking, swimming, and water walking are frequently suggested because they are gentle on joints and increase blood and lymph circulation in impaired extremities. These exercises can decrease pain, minimize inflammation, and facilitate movement through everyday life.
For instance, water aerobics leverages buoyancy to alleviate the weight of the body, making movement less painful and more fun for those with lipedema. Choose activities that feel good and can be sustained. Consistency is more important than intensity.

Whether it’s a walk around the block, a light stretching routine, or some simple yoga, you can do these most days and they will help symptoms such as heaviness and aching. Even small victories like walking a little further each week can improve moods and make daily activities less overwhelming.
Lipedema warriors need to stop being a hero and learn to actually listen to their bodies and not push so hard. Exercising or lifting heavy things too much can cause greater pain and inflammation. The aim is consistent, light motion, not intense exercise.
Others swear by rubbing in healing creams like arnica or CBD oil on achy spots to stay mobile. Physical therapists could be a godsend. They understand how to design safe, customized workouts that suit each individual’s abilities and restrictions.
This support aids in persistence, making it easier to stay with movement and witness progress over time.
Compression Therapy
Compression therapy is yet another lipedema swelling and pain management tool. It helps shift lymphatic fluid and reduces pain, particularly when combined with light movement.
Compression Therapy Checklist:
- Opt for the right fit and strength of compression garments (stockings, sleeves).
- Wear them as recommended, typically throughout the day and when moving.
- Include pneumatic pump sessions lasting 30 to 60 minutes to assist in pumping fluid out of the legs.
- Examine skin every day for indications of irritation or pressure marks.
- Wash and replace garments as recommended to maintain effectiveness.
Compression therapy frequently and in a daily regimen might provide improved outcomes. It is ideal to work with an expert to identify the appropriate products and develop a plan that matches your lifestyle and symptoms.
Advanced Therapies
Advanced therapies for lipedema aim to relieve symptoms and tackle swelling that doesn’t subside with diet or exercise. These treatments are both non-surgical and surgical in nature, each playing its part. Many individuals discover that a combination of therapies offers the most effective outcome.
Partnering with a care team that knows lipedema is critical to receiving quality care and monitoring progress. Other alternatives might work better for different individuals, so trying out these treatments with assistance from reliable healthcare providers is crucial.
Decongestive Therapy
Decongestive therapy seeks to decrease swelling and pain in the legs through specialized techniques to assist the lymph system in removing fluid from the tissues. Manual lymph drainage, compression bandaging, skin care, and light exercise are often part of this therapy. These measures combine to support decongestion and reduce the possibility of skin complications.
Manual lymph drainage is a light massage that directs lymph fluid away from swollen areas to regions where it can drain more effectively. This can help the legs feel lighter and looser. Compression wraps or stockings provide consistent pressure, which prevents further fluid accumulation and keeps the swelling down once it’s gone.
Patients need to consider decongestive therapy as an important weapon in their arsenal, not a band-aid solution. It’s compatible with other therapies and healthy habits for a more comprehensive approach. This is where trained specialists, such as certified lymphedema therapists, come in. The proper technique is not just important for safety, but for the results.
Surgical Options
Surgery is an option for some lipedema patients when non-surgical alternatives fail to manage pain, swelling, or mobility concerns. The most common surgical approach is tumescent liposuction, which removes abnormal fat deposits while attempting to spare lymph vessels. Water-assisted liposuction and laser-assisted liposuction are utilized by certain clinics.
These surgeries can reduce lower limb size, relieve pain, and increase mobility. However, outcomes are inconsistent.
| Surgery Type | Method Used | Typical Benefits | Possible Risks |
|---|---|---|---|
| Tumescent Liposuction | Saline solution + suction | Fat reduction, better movement | Swelling, bruising, infection |
| Water-Assisted Liposuction | Jet of water to loosen fat | Less tissue damage, quick recovery | Nerve injury, uneven results |
| Laser-Assisted Liposuction | Laser energy to melt fat | Skin tightening, fat removal | Burns, fluid buildup |
Contemplating surgery is a significant decision. Everyone should discuss it candidly with their physicians, be inquisitive, and balance the potential benefits and dangers. Selecting a surgeon who is renowned for their skill in lipedema care is key for a safer experience and better results.
The Mental Weight
Lipedema life can be heavy, both physically and mentally. Even hardcore diet and exercise regimens seem to have no effect on the shape or size of their legs. This can be hard to bear and adds to the stress of managing a chronic condition. Dealing with the mental weight is just as crucial as the physical. Emotional well-being, community, and counseling are important aspects of comprehensive care for lipedema.
Emotional Impact
Frustration arises when fat-loss efforts fail to impact the areas most affected by lipedema. Many patients report feeling dismissed by friends, family, or even physicians who recommend that more willpower or stricter diets may help. This cyclical message breeds melancholy and self-loathing, and it’s why the illness is so difficult to discuss openly.
To escape nosy commentary or interrogations, others retreat from social occasions. Learning to be kind to yourself in these moments is essential. Acknowledging the things that cannot be altered immediately can lighten some of the mental burden. A self-compassionate individual might be more forgiving when faced with setbacks or slow progress.
Opening up with others about what you really think and feel can assist as well. Open dialog about mental health in the lipedema community creates an opportunity for genuine support. When people disclose their stories, it can make others feel less isolated. Others discover that therapy or counseling provides room to work through their emotions.
For example, cognitive behavioral therapy (CBT) can help challenge negative thinking patterns and build healthy coping skills.
Building Resilience
Resilience, which is the capacity to rebound from hard circumstances, is a muscle that strengthens with use. Lipedema warriors will encounter setbacks or slow growth, but cultivating resiliency allows them to continue advancing. It is good to establish achievable goals, such as remaining physically active or attending medical appointments.
When you achieve these goals, basking in the glory of the little victories can provide an upsurge in self-esteem and motivation. A good attitude doesn’t imply sucking up genuine issues. Focus on the mental weight, which is to say focusing on finding ways to evolve, even through difficult times.
Having friends and family support, or connecting with others with lipedema, can make a big difference here. Self-care rituals — short walks, stretching, quiet time — can help mitigate this stress. Other practices, like mindfulness or journaling, can provide relief.
Over time, these habits accumulate and contribute to better mood and quality of life.
Conclusion
Lipedema legs won’t shrink with dieting. These lipedema legs don’t shrink with dieting; they stay swollen and sore, no matter how much you cut calories. Health is more than just your scale info. Food and gentle exercise make your body feel better, but they won’t make the fat disappear. Others require specific treatment, such as therapy or surgery. The brain needs nurturing as well. They hide shame or stress that doesn’t appear on the surface. Support means the world. Speaking out and seeking assistance can take some of the burden off your heart. To discover more or get the right care, contact a health professional. No one ever has to navigate lipedema by themselves.
Frequently Asked Questions
Why don’t lipedema legs shrink with dieting?
Lipedema legs won’t diet away. Lipedema legs won’t shrink with dieting and exercise because the fat is due to a chronic condition, not just calorie intake.
Is lipedema just regular fat?
No, lipedema fat is different from normal fat. It builds up disproportionally and is frequently painful or sensitive. This fat does not respond well to diet or exercise.
Can lipedema be cured by losing weight?
Lipedema legs don’t shrink with dieting. Eating on the healthy side can aid, but targeted treatments are required for lipedema symptoms and fat deposits.
What treatments help lipedema legs?
Lipedema is treated with things like manual lymphatic drainage, compression garments, and special surgeries. You need professional advice for optimal outcomes.
How can movement help with lipedema?
STAGE 1: Gentle activity, like walking or swimming, promotes lymphatic circulation and alleviates ache. You don’t even need high-impact exercise. Light activity may control symptoms but will not rid you of lipedema fat.
Is lipedema related to being overweight?
Lipedema is a disease, not overweight. Any body type can have lipedema. Lipedema legs won’t shrink with dieting.
Can diet changes help with lipedema symptoms?
A well-balanced diet can aid your overall health and help fight inflammation. It doesn’t remove lipedema fat. Medical treatment is advised for symptoms.